CATHETERIZATION: A COMPREHENSIVE GUIDE
- INTRODUCTION
Definition
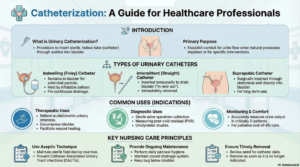
Urinary catheterization is a medical procedure involving the insertion of a hollow, flexible tube (catheter) into the urinary bladder through the urethra for the purpose of draining urine, measuring output, or instilling medications (Potter & Perry, 2021).
Historical Background
- Ancient times: Hollow reeds and metal tubes were used
- 1853: Jean François Reybard introduced rubber catheters
- 1930s: Frederic Foley developed the self-retaining balloon catheter
- Modern era: Silicone and hydrogel-coated catheters developed
Anatomy Review
Understanding the urinary system anatomy is essential:
- Female urethra: 3-4 cm long
- Male urethra: 18-20 cm long
- Bladder capacity: 300-500 ml in adults
- TYPES OF CATHETERIZATION
- Based on Duration
- Intermittent (In-and-Out) Catheterization
- Single-use catheter inserted to empty bladder
- Removed immediately after drainage
- Duration: Few minutes only
- Indwelling (Retention) Catheterization
- Remains in place for extended periods
- Secured by inflation balloon
- Duration: Days to weeks
- Suprapubic Catheterization
- Inserted through abdominal wall
- Directly into bladder
- Surgical procedure required
- Based on Catheter Material
| Material | Duration | Characteristics |
| Latex | Short-term (up to 14 days) | Flexible, inexpensive, allergy risk |
| Silicone | Long-term (up to 12 weeks) | Hypoallergenic, rigid |
| Teflon-coated | Medium-term (up to 28 days) | Reduced friction |
| Hydrogel-coated | Long-term | Biocompatible, comfortable |
| Silver-alloy coated | Long-term | Antimicrobial properties |
| PVC | Short-term/Intermittent | Disposable, economical |
- Types of Catheters
- Foley Catheter (Indwelling)
- Description: Double/triple lumen with retention balloon
- Balloon sizes: 5-30 ml
- French sizes: 12-24 Fr (adults)
- Uses: Continuous drainage
- Straight/Robinson Catheter
- Description: Single lumen, no balloon
- Uses: Intermittent catheterization
- Material: Usually plastic or rubber
- Coudé Catheter
- Description: Curved/angled tip
- Uses: Enlarged prostate, urethral strictures
- Special feature: Facilitates passage past obstruction
- Three-Way (Triple Lumen) Catheter
- Description: Three channels
- Drainage
- Balloon inflation
- Irrigation
- Uses: Continuous bladder irrigation, post-TURP
- Nelaton Catheter
- Description: Straight tip, single lumen
- Uses: Intermittent catheterization
- Material: Flexible rubber
- Malecot Catheter
- Description: Wing-tip design
- Uses: Suprapubic drainage
- Pezzer Catheter
- Description: Mushroom-shaped tip
- Uses: Suprapubic drainage
- Catheter Sizes
French Scale (Fr): Circumference in millimeters
| Patient Category | Recommended Size |
| Adult Female | 14-16 Fr |
| Adult Male | 16-18 Fr |
| Children | 8-10 Fr |
| Infants | 5-6 Fr |
| Post-operative/Hematuria | 20-24 Fr |
- USES AND INDICATIONS
- Therapeutic Indications
- Urinary Retention
- Acute retention
- Chronic retention
- Neurogenic bladder
- Urinary Obstruction
- Benign prostatic hyperplasia
- Urethral strictures
- Blood clots
- Perioperative Management
- Major surgical procedures
- Pelvic/urological surgeries
- Prolonged anesthesia
- Bladder Irrigation
- Post-prostatectomy
- Clot evacuation
- Medication instillation
- Incontinence Management
- Severe skin breakdown
- Patient comfort (end-of-life care)
- Diagnostic Indications
- Accurate Urine Output Monitoring
- Critically ill patients
- Shock management
- Fluid resuscitation
- Specimen Collection
- Sterile urine sample
- Culture and sensitivity
- When clean-catch not possible
- Diagnostic Procedures
- Cystography
- Urodynamic studies
- Residual urine measurement
- Contraindications
Absolute:
- Urethral trauma/injury
- Known urethral stricture (without specialist)
- Recent urethral surgery
Relative:
- Urinary tract infection
- Coagulopathy
- Latex allergy (use silicone)
- NURSING CARE
- Pre-Procedure Care
- Assessment
- Medical history review
- Previous catheterization
- Allergies (latex, antiseptics)
- Urological conditions
- Recent surgeries
- Physical assessment
- Genital area inspection
- Signs of infection
- Anatomical abnormalities
- Cognitive status
- Patient Preparation
- Explanation and consent
- Procedure description
- Purpose and duration
- Potential complications
- Answer questions
- Privacy and comfort
- Draw curtains/close door
- Proper lighting
- Comfortable positioning
- Emotional support
- Equipment Preparation
Catheterization Tray Contents:
- Sterile gloves (2 pairs)
- Sterile drapes (fenestrated and plain)
- Antiseptic solution (povidone-iodine/chlorhexidine)
- Cotton balls/gauze
- Sterile lubricant (water-soluble)
- Appropriate catheter
- Sterile syringe with water
- Urine collection bag
- Specimen container
- Forceps
- Procedure (Nursing Responsibilities)
Female Catheterization
Positioning:
- Supine with knees flexed
- Feet flat, knees apart (dorsal recumbent)
- Adequate lighting
Steps:
- Perform hand hygiene
- Don sterile gloves
- Create sterile field
- Cleanse perineum (front to back)
- Separate labia with non-dominant hand
- Identify urethral meatus
- Cleanse urethral meatus (single strokes)
- Insert lubricated catheter (5-7.5 cm)
- Advance until urine flows
- Inflate balloon with sterile water
- Gently pull back to seat balloon
- Secure catheter to inner thigh
Male Catheterization
Positioning:
- Supine with legs extended
- Or slightly abducted
Steps:
- Perform hand hygiene
- Don sterile gloves
- Create sterile field
- Hold penis at 90-degree angle
- Retract foreskin (if uncircumcised)
- Cleanse glans in circular motion
- Insert lubricated catheter (17-22.5 cm)
- Advance until urine flows
- Advance additional 2.5-5 cm
- Inflate balloon
- Replace foreskin
- Secure to lower abdomen
- Post-Procedure Care
- Immediate Care
- Document procedure details
- Record initial urine output
- Assess patient comfort
- Ensure proper drainage
- Ongoing Assessment
| Parameter | Frequency | Documentation |
| Urine output | Hourly (ICU) or every 4-8 hours | Volume, color, clarity |
| Catheter patency | Every shift | Kinks, blockages |
| Insertion site | Daily | Redness, discharge |
| Balloon integrity | Daily | Proper placement |
| Patient comfort | Every shift | Pain, discomfort |
- Daily Catheter Care
Meatal Care Protocol:
- Clean with soap and water daily
- Clean after bowel movements
- No routine antiseptic application
- Maintain downward drainage
- Secure catheter properly
- Infection Prevention Bundle (CAUTI Bundle)
Evidence-based interventions:
- Avoid unnecessary catheterization
- Use aseptic insertion technique
- Maintain closed drainage system
- Remove catheter promptly when no longer needed
- Daily assessment of catheter necessity
- Catheter Maintenance
Drainage Bag Management
- Keep below bladder level
- Never place on floor
- Empty when 2/3 full
- Use separate container for each patient
- Avoid breaking closed system
Preventing Complications
- Encourage fluid intake (if not contraindicated)
- Avoid tension on catheter
- Monitor for signs of UTI
- Regular position changes
- Perineal hygiene
- Catheter Removal
Indications for Removal
- No longer medically necessary
- Blocked catheter requiring replacement
- Patient request (with physician order)
- Evidence of infection
Procedure
- Explain procedure to patient
- Deflate balloon completely
- Ask patient to breathe deeply
- Gently withdraw catheter
- Dispose properly
- Document time of removal
- Monitor voiding within 6-8 hours
Post-Removal Monitoring
- First void timing
- Urine amount
- Dysuria
- Urinary retention signs
- Bladder scanning if needed
- COMPLICATIONS
- Immediate Complications
| Complication | Cause | Prevention |
| Trauma/Bleeding | Forceful insertion | Gentle technique, adequate lubrication |
| False passage | Wrong direction | Proper anatomy knowledge |
| Paraphimosis | Unreturned foreskin | Always return foreskin |
| Balloon inflation in urethra | Early inflation | Wait for urine flow |
- Long-term Complications
- Catheter-Associated UTI (CAUTI)
- Most common complication
- Risk increases 3-7% per day
- Preventable with bundle approach
- Urethral Stricture
- Due to repeated catheterization
- Larger catheter sizes
- Bladder Stones
- Long-term catheterization
- Encrustations
- Urethral Erosion
- Improper securing
- Prolonged use
- Catheter Blockage
- Sediment accumulation
- Blood clots
- Signs Requiring Immediate Attention
- No urine drainage
- Bypassing around catheter
- Fever/chills
- Cloudy/foul-smelling urine
- Hematuria
- Bladder spasms
- Abdominal pain
- SPECIAL CONSIDERATIONS
- Pediatric Catheterization
- Smaller catheter sizes (5-10 Fr)
- Extra gentleness required
- Parental presence consideration
- Age-appropriate explanation
- Play therapy preparation
- Geriatric Catheterization
- Assess for prostatic enlargement
- Consider decreased mobility
- Skin fragility
- Cognitive impairment considerations
- Higher infection risk
- Patient Education
- Purpose of catheter
- Care of catheter and bag
- Signs of complications
- When to seek help
- Activity modifications
- DOCUMENTATION
Essential elements to document:
- Date and time
- Indication for catheterization
- Catheter type and size
- Balloon inflation volume
- Amount and characteristics of urine
- Patient tolerance
- Any difficulties encountered
- Patient education provided
REFERENCES
- Potter, P. A., Perry, A. G., Stockert, P. A., & Hall, A. M. (2021). Fundamentals of Nursing (10th ed.). Elsevier.
- Taylor, C., Lillis, C., Lynn, P., & LeMone, P. (2020). Fundamentals of Nursing: The Art and Science of Person-Centered Care (9th ed.). Wolters Kluwer.
- Brunner, L. S., & Suddarth, D. S. (2020). Brunner & Suddarth’s Textbook of Medical-Surgical Nursing (14th ed.). Wolters Kluwer.
- Centers for Disease Control and Prevention. (2019). Guideline for Prevention of Catheter-Associated Urinary Tract Infections. CDC.
- Gould, C. V., Umscheid, C. A., Agarwal, R. K., Kuntz, G., & Pegues, D. A. (2019). Healthcare Infection Control Practices Advisory Committee. HICPAC Guidelines for Prevention of CAUTI. Infection Control & Hospital Epidemiology, 40(1), 1-52.
- Loveday, H. P., Wilson, J. A., Pratt, R. J., et al. (2014). Epic3: National Evidence-Based Guidelines for Preventing Healthcare-Associated Infections. Journal of Hospital Infection, 86(Suppl 1), S1-S70.
- National Institute for Health and Care Excellence (NICE). (2020). Healthcare-associated infections: prevention and control in primary and community care. NICE Clinical Guidelines.
- Dougherty, L., & Lister, S. (2015). The Royal Marsden Manual of Clinical Nursing Procedures (9th ed.). Wiley-Blackwell.
- American Nurses Association. (2021). Streamlined Evidence-Based RN Tool: Catheter Associated Urinary Tract Infection (CAUTI) Prevention. ANA.
- Hooton, T. M., Bradley, S. F., Cardenas, D. D., et al. (2010). Diagnosis, Prevention, and Treatment of Catheter-Associated Urinary Tract Infection in Adults. Clinical Infectious Diseases, 50(5), 625-663.
