Diverticulosis and Diverticulitis:
Introduction of Diverticulosis – Diverticulitis : Understanding the distinction between these two conditions (Diverticulosis and Diverticulitis ) is essential; it can be compared to identifying a weak spot on a tire.
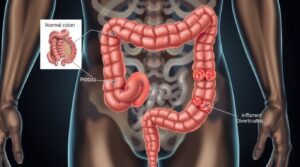
Above Image Generated by AI (for educational Purpose only)
-
Diverticulosis: The weak spots have formed (the diverticula), but the tire is still holding air and functioning. This is the structural condition.Definition of Diverticulosis: A condition characterized by the presence of diverticula (small, bulging pouches or sacs) that develop in the lining of the digestive system, most commonly in the sigmoid colon (the lower part of the large intestine).
-
Diverticulitis: One of those weak spots has become inflamed or infected, like a blister on the tire that is about to burst. This is the acute inflammatory condition. Definition of Diverticulitis : The inflammation or infection of one or more diverticula. This occurs when these pouches become blocked with stool or undigested food, leading to bacterial overgrowth, inflammation, and potential perforation.
Click Here to Buy👉 Digestive Enzymes Postbiotics Prebiotics Probiotics for Women & Men
Common Etiology (Causes) :
-
Low-fiber diet (leading to constipation and increased colon pressure)
-
Aging – decreased muscle tone in the colon wall
-
Chronic constipation
-
Obesity
-
Sedentary lifestyle
-
Genetic predisposition
-
Use of NSAIDs or corticosteroids (can irritate colon wall)
Pathophysiology
-
In Diverticulosis, high intraluminal pressure pushes mucosa and submucosa through weak areas of the muscular layer → formation of diverticula.
-
Retention of fecal matter or undigested food in these diverticula leads to obstruction, causing bacterial overgrowth and inflammation (Diverticulitis).
-
The inflamed diverticulum can cause localized abscesses, perforation, peritonitis, or fistula formation in severe cases.
Clinical Manifestations
Diverticulosis (often asymptomatic)
-
Mild abdominal discomfort
-
Bloating, constipation, or irregular bowel habits
-
Cramping in the lower left quadrant
Diverticulitis (symptomatic phase)
-
Left lower quadrant pain (most common)
-
Fever and chills
-
Nausea and vomiting
-
Abdominal tenderness or guarding
-
Changes in bowel habits (constipation or diarrhea)
-
Possible rectal bleeding
Click Here to Buy👉 Digestive Enzymes Postbiotics Prebiotics Probiotics for Women & Men
Diagnostic Evaluation:
-
Physical Examination: Abdominal tenderness (LLQ)
-
Laboratory Tests:
-
CBC – ↑ WBC count (infection)
-
ESR/CRP – elevated in inflammation
-
-
Imaging:
-
CT Scan (most definitive) – shows inflamed or perforated diverticula
-
Ultrasound – to rule out abscess
-
Colonoscopy (after inflammation subsides) – to assess diverticula extent
-
-
Stool Examination: To check for occult blood
Medical Management
For Diverticulosis:
-
High-fiber diet (whole grains, fruits, vegetables)
-
Adequate fluid intake
-
Avoidance of constipation (bulk-forming laxatives if needed)
-
Regular exercise
For Diverticulitis (Acute phase):
-
Bowel Rest: NPO → clear liquid diet → low-fiber → high-fiber gradually
-
Antibiotics: Broad-spectrum (e.g., Metronidazole, Ciprofloxacin)
-
IV Fluids: Maintain hydration and electrolyte balance
-
Pain management: Analgesics (Avoid NSAIDs)
-
Surgery (if complications occur):
-
Abscess drainage
-
Bowel resection (if perforation, peritonitis, or fistula)
-
Nursing Care Plan for Diverticulitis
Nursing Diagnosis 1: Acute Pain related to inflammation and infection of diverticula.
-
Desired Outcomes:
-
Patient reports pain reduction to a tolerable level (e.g., 3/10 on a 0-10 scale).
-
Patient demonstrates relaxed body posture and participates in activities as tolerated.
-
Vital signs (heart rate, blood pressure) are within the patient’s normal limits.
-
-
Nursing Interventions:
-
Assessment:
-
Assess pain characteristics (location, intensity, quality, duration, aggravating/alleviating factors) using a pain scale.
-
Monitor vital signs regularly, noting any increases related to pain.
-
Observe for nonverbal cues of pain (restlessness, grimacing, guarding).
-
-
Intervention:
-
Administer prescribed analgesics (e.g., opioids for severe pain, acetaminophen for mild) as ordered, and evaluate their effectiveness. Avoid NSAIDs as they can increase the risk of perforation.
-
Provide non-pharmacological pain relief measures:
-
Apply a warm compress to the abdomen (unless contraindicated).
-
Encourage relaxation techniques (deep breathing, guided imagery).
-
Provide a comfortable environment (quiet, dim lighting).
-
-
Ensure bowel rest as ordered (NPO, clear liquids), which can reduce pain by decreasing colonic spasms.
-
Assist with repositioning to a comfortable position, often semi-Fowler’s.
-
-
Education:
-
Educate the patient on medication use, side effects, and when to report uncontrolled pain.
-
Teach relaxation techniques.
-
-
Nursing Diagnosis 2: Risk for Infection related to inflammation of diverticula and potential for perforation/abscess formation.
-
Desired Outcomes:
-
Patient remains free of signs and symptoms of worsening infection (e.g., fever, chills, increased WBC, purulent drainage).
-
Patient demonstrates understanding of antibiotic therapy.
-
-
Nursing Interventions:
-
Assessment:
-
Monitor vital signs frequently, particularly temperature, for signs of fever.
-
Monitor complete blood count (CBC) for elevated white blood cell (WBC) count, indicating infection.
-
Assess for increasing abdominal tenderness, rigidity, or rebound tenderness, which could indicate peritonitis.
-
Monitor for signs of abscess formation (localized swelling, persistent fever).
-
-
Intervention:
-
Administer prescribed antibiotics on time and ensure completion of the full course.
-
Maintain strict aseptic technique during all invasive procedures (e.g., IV insertion, catheter care).
-
Monitor intake and output, and ensure adequate hydration through IV fluids as ordered.
-
Prepare for possible diagnostic tests (e.g., repeat CT scan) if symptoms worsen.
-
If an abscess is present, prepare for or assist with percutaneous drainage.
-
If surgical intervention is required, provide pre- and post-operative care (e.g., wound care, stoma care if an ostomy is formed).
-
-
Education:
-
Educate the patient on the importance of completing the full course of antibiotics, even if feeling better.
-
Instruct on signs and symptoms of worsening infection to report immediately.
-
-
Nursing Diagnosis 3: Deficient Knowledge related to disease process, dietary management, and prevention of recurrence.
-
Desired Outcomes:
-
Patient verbalizes understanding of diverticulosis/diverticulitis, its causes, and treatment.
-
Patient identifies appropriate dietary modifications for acute and chronic phases.
-
Patient verbalizes strategies to prevent recurrence (e.g., high-fiber diet, hydration, exercise).
-
-
Nursing Interventions:
-
Assessment:
-
Assess the patient’s current knowledge level regarding the disease.
-
Identify learning barriers (e.g., pain, anxiety, language).
-
-
Intervention:
-
Explain diverticulosis and diverticulitis in simple, understandable terms.
-
Discuss the importance of a clear liquid diet during acute flare-ups and gradual progression to a low-fiber diet, then eventually a high-fiber diet once inflammation subsides.
-
Provide detailed instructions on a high-fiber diet:
-
Emphasize gradual increase in fiber intake to avoid bloating and gas.
-
Recommend foods rich in fiber (fruits, vegetables, whole grains, legumes).
-
Explain the role of fiber supplements if dietary intake is insufficient.
-
-
Stress the importance of adequate fluid intake (at least 8 glasses of water daily) to prevent constipation and facilitate fiber’s effectiveness.
-
Advise regular physical activity to promote bowel motility.
-
Discuss the role of avoiding straining during bowel movements.
-
Explain the importance of reporting new or worsening symptoms to a healthcare provider.
-
Clarify common misconceptions (e.g., that nuts, seeds, and popcorn always cause flare-ups – current evidence suggests this is not true for most people, but individual tolerance varies).
-
-
Education:
-
Provide written educational materials for reinforcement.
-
Encourage questions and provide opportunities for clarification.
-
Involve family members or significant others in education as appropriate.
-
-
Nursing Diagnosis 4: Imbalanced Nutrition: Less Than Body Requirements related to bowel rest, decreased intake, and potential malabsorption.
-
Desired Outcomes:
-
Patient maintains adequate hydration and electrolyte balance.
-
Patient demonstrates progressive tolerance to diet as ordered.
-
Patient verbalizes understanding of dietary progression.
-
-
Nursing Interventions:
-
Assessment:
-
Monitor patient’s hydration status (skin turgor, mucous membranes, urine output, vital signs).
-
Monitor electrolyte levels (sodium, potassium, chloride).
-
Assess tolerance to dietary progression (presence of nausea, vomiting, abdominal pain, distension, diarrhea).
-
-
Intervention:
-
Administer IV fluids as prescribed to maintain hydration and electrolyte balance during bowel rest.
-
Follow prescribed dietary progression (e.g., NPO → clear liquids → full liquids → low-fiber diet → high-fiber diet).
-
Offer small, frequent meals as diet advances to improve tolerance.
-
Encourage sips of water or ice chips during NPO status if permitted.
-
Consult with a dietitian for individualized meal planning and nutritional support.
-
-
Education:
-
Explain the rationale for dietary restrictions and progression.
-
Educate on identifying foods that may exacerbate symptoms.
-
Emphasize the importance of adequate nutrition for healing.
-
-
Nursing Care Plan for Diverticulitis:
| Nursing Diagnosis | Expected Outcomes (SMART Goals) | Nursing Interventions | Health Teaching |
| Acute Pain related to inflammation and infection of diverticula | – Patient reports pain reduction to a tolerable level (e.g., 3/10 on a 0-10 scale) within 24-48 hours. <br> – Patient demonstrates relaxed body posture and uses non-pharmacological methods for pain relief within 24 hours. <br> – Vital signs remain within patient’s normal limits within 24-48 hours. | – Assess pain characteristics (PQRST, scale 0-10) and vital signs every 2-4 hours. <br> – Administer prescribed analgesics (avoiding NSAIDs) and evaluate effectiveness within 30-60 minutes. <br> – Provide non-pharmacological interventions: warm compresses, relaxation techniques (deep breathing, guided imagery), comfortable positioning. <br> – Ensure bowel rest (NPO/clear liquids) as ordered. <br> – Provide a quiet, comfortable environment. | – Explain medication purpose, dosage, schedule, and potential side effects. <br> – Emphasize reporting uncontrolled pain or new symptoms. <br> – Teach and reinforce relaxation techniques. <br> – Advise against using NSAIDs for pain relief. |
| Risk for Infection related to inflammation of diverticula and potential for perforation/abscess formation | – Patient remains free of signs and symptoms of worsening infection (e.g., fever < 38°C, WBC count within normal range, absence of purulent drainage, no increased abdominal tenderness) throughout hospitalization. <br> – Patient verbalizes understanding of antibiotic therapy and necessity of completion prior to discharge. | – Monitor vital signs, especially temperature, every 2-4 hours. <br> – Monitor CBC for elevated WBC count daily. <br> – Assess abdomen for increasing tenderness, rigidity, rebound tenderness, or localized swelling every 4 hours. <br> – Administer prescribed antibiotics on time and ensure full course completion. <br> – Maintain strict aseptic technique for all invasive procedures. <br> – Monitor intake and output, ensure adequate hydration (IV fluids as ordered). <br> – Prepare for/assist with diagnostic tests (e.g., repeat CT) or interventions (e.g., abscess drainage, surgery). | – Explain the importance of completing the full course of antibiotics, even if symptoms improve. <br> – Instruct on signs and symptoms of worsening infection (fever, chills, increased pain, pus) to report immediately. <br> – Emphasize hand hygiene to prevent spread of infection. |
| Deficient Knowledge related to disease process, dietary management, and prevention of recurrence | – Patient verbalizes understanding of diverticulosis/diverticulitis, causes, and treatment plan by discharge. <br> – Patient identifies appropriate dietary modifications for acute and chronic phases by discharge. <br> – Patient verbalizes at least three strategies to prevent recurrence (e.g., high-fiber diet, hydration, exercise) by discharge. | – Assess current knowledge level and learning barriers. <br> – Explain the disease process (diverticula formation, inflammation) in simple terms. <br> – Discuss dietary progression: acute (clear liquids), recovery (low-fiber), long-term (high-fiber). <br> – Provide detailed guidance on increasing fiber intake gradually: fruits, vegetables, whole grains, legumes. <br> – Emphasize adequate fluid intake (8+ glasses/day) and regular exercise. <br> – Clarify common misconceptions about nuts/seeds. <br> – Discuss importance of avoiding straining during bowel movements. <br> – Explain signs and symptoms warranting immediate medical attention. | – Provide written educational materials on diet (foods to include/avoid), fluid intake, and exercise. <br> – Teach gradual increase of fiber and the need for ample fluids with fiber. <br> – Encourage active participation in discharge planning. <br> – Advise on symptom recognition and when to seek medical care. <br> – Involve family in teaching as appropriate. |
| Imbalanced Nutrition: Less Than Body Requirements related to bowel rest, decreased intake, and potential malabsorption | – Patient maintains adequate hydration and electrolyte balance as evidenced by stable vital signs, good skin turgor, and balanced intake/output within 48-72 hours. <br> – Patient tolerates prescribed dietary progression without nausea, vomiting, or increased abdominal pain prior to discharge. <br> – Patient verbalizes understanding of the rationale for dietary restrictions and progression by discharge. | – Monitor hydration status (skin turgor, mucous membranes, I&O, daily weights) and electrolyte levels. <br> – Administer IV fluids as prescribed. <br> – Follow prescribed dietary progression strictly (NPO → clear liquids → full liquids → low-fiber → high-fiber). <br> – Offer small, frequent meals as diet advances to improve tolerance. <br> – Assess for tolerance to diet changes (nausea, vomiting, distension, pain, diarrhea). <br> – Consult with a dietitian for individualized nutritional planning. | – Explain the rationale behind diet progression and the importance of adhering to it to allow the bowel to rest and heal. <br> – Teach the patient how to identify foods that may trigger symptoms. <br> – Encourage patient to eat slowly and chew food thoroughly. <br> – Emphasize the importance of adequate nutrition for healing and recovery. |
